Malignant Infantile Osteopetrosis with Rickets: A Rare Paradoxical Association
Maria Hassan
Department of Radiology, Dr. Ziauddin Hospital, Karachi, Pakistan
- Corresponding Author:
- Maria Hassan
Department of Radiology
Dr. Ziauddin Hospital, Karachi, Pakistan
Tel: 923333175721
E-mail: misshassan07@hotmail.com
Received date: December 12, 2019; Accepted date: February 19, 2020; Published date: February 26, 2020
Citation: Hassan M (2020) Malignant Infantile Osteopetrosis with Rickets: A rare Paradoxical Association. J Prev Med Vol. 5 Iss No. 1: 4.
Copyright:© 2020 Hassan M. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A rare congenital disorder of bone resorption is Malignant Infantile Osteopetrosis. It is caused by failure of osteoclasts to reabsorb immature bone. Malignant infantile osteopetrosis is present at birth or develops within the first few months of life. We are reporting a case of a child who presented to us with pain and swelling in left thigh. He was diagnosed as malignant infantile osteopetrosis with rickets, which is a rare paradoxical association.
Keywords
Malignant; Infantile osteopetrosis; Rickets
Introduction
Osteopetrosis is a rare congenital disorder that makes bones abnormally dense and prone to breakage. The different types of osteopetrosis are distinguished by their pattern of inheritance as autosomal dominant, autosomal recessive, or Xlinked.
Albers-Schönberg disease which is Autosomal Dominant Osteopetrosis (ADO), is typically the mildest type of the disorder and may be asymptomatic or symptomatic. In asymptomatic patients, the unusually dense bones may be revealed incidentally when an x-ray is performed for another reason.
Symptomatic patients usually present in late childhood or adolescence with major features of the condition include multiple bone fractures, arthritis in the hips, osteomyelitis, scoliosis or other spinal abnormalities. Autosomal Recessive Osteopetrosis (ARO), also called malignant infantile osteopetrosis is a more severe form of the disorder that becomes apparent in early infancy.
These patients are prone to bone fracture even from minor bumps and falls. They have abnormally dense skull bones with narrowing of neural foramina at the skull base and resultant vision and hearing loss, as well as paralysis of facial muscles. Dense bones also impair medullary hematopoiesis; as a result, people with severe osteopetrosis are at risk of abnormal bleeding, anemia, and recurrent infections.
Life threatening complication is bone marrow suppression which can be life threatening presenting in infancy and early childhood [1]. Rickets is a rare paradoxical complication of malignant infantile osteopetrosis because in children with osteopetrosis there is positive total body calcium balance [2].
Other features include slow growth and short stature, hepatosplenomegaly, tooth eruption and other dental abnormalities. A rare type of inheritance is X-linked. In this form, in addition to abnormally dense bones, accumulation of fluid resulting in lymphedema and a condition that affects the skin, hairs, teeth, and sweat glands called anhydrotic ectodermal dysplasia is identified [1].
Case Description
A four-month-old baby girl, younger sibling of two, born out of consanguineous marriage presented to the emergency department with complaints of left thigh swelling and pain. There was no history of any witnessed trauma or any known co-morbids. The birth history was insignificant and all developmental milestones were appropriate for age.
Physical examination revealed a pale child with short stature, frontal bossing and wide-open anterior fontanelle. Abdomen was distended with hepatomsplenomegaly. Rest of the systemic examination was unremarkable. Biochemical investigations showed anemia, hypocalcaemia, hypophosphetemia and high serum alkaline phosphatase.
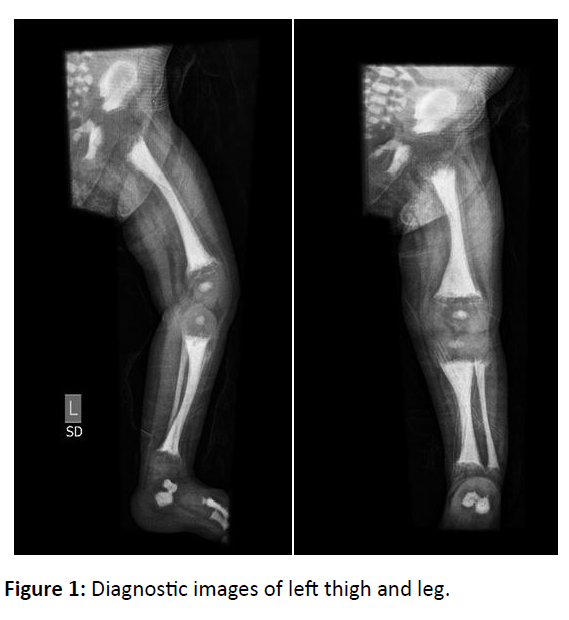
X-ray showed spiral fracture of proximal diaphysis of left femur with periosteal reaction. Diffuse sclerosis with loss of cortico-medullary distinction was seen in all the visualized bones. Widening, cupping and fraying of proximal and distal metaphysis of left femur, tibia and fibula was noted.
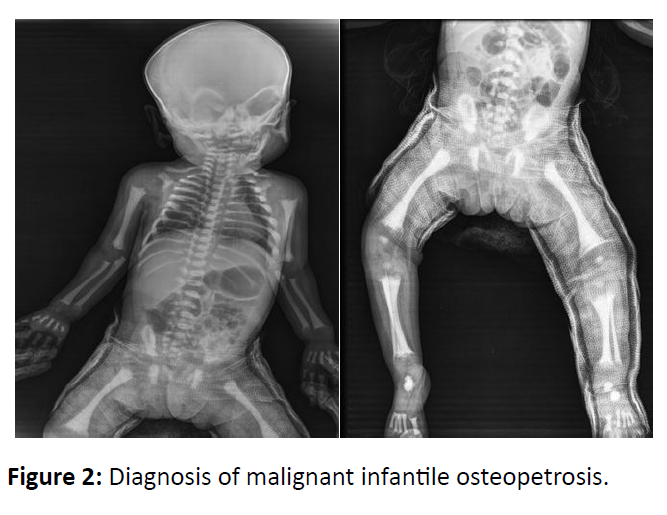
Patient was recalled for complimentary baby gram, which showed similar appearance in all bones. Hence, the diagnosis of Malignant Infantile Osteopetrosis with super imposed rickets was confirmed (Figures 1 and 2).
Discussion
Osteopetrosis is a rare severe genetic disorder due to abnormal osteoclast activity [3]. It is more common in consanguineous populations. Four types of osteopetrosis have been described. Autosomal recessive or malignant infantile type presents at birth or early infancy. Based on the clinical history and radiographic findings, the child was diagnosed having infantile or malignant type of osteopetrosis with superimposed rickets. Its characteristic feature is rickets, which results from the defective osteoclasts failing to provide normal calcium and phosphorus balance resulting in the poor mineralization of the osteoid [4].
The increase in bone density in osteopetrosis weakens the bone, making it prone to fractures, which is a common initial presenting symptom [5]. A characteristic radiological feature seen was generalized increase in bone density, with a loss of cortico-medullary distinction. Visual and hearing impairment and facial paralysis resulting from bony encroachment of the neural foramina can also be identified. Hematological manifestations associated with osteopetrosis include severe anemia and hepatosplenomegaly. The hypersplenism in return leads to thrombocytopenia, leukopenia and hemolytic anemia.
It is imperative to diagnose association of rickets with osteopetrosis due to two main reasons- foremost treatment of rickets improves child's activity, increases appetite, decreases irritability and protects the child from recurrent respiratory tract infections; secondly, treatment of rickets is essential for best treatment results with bone marrow transplantation (BMT), if available. Treatment of rickets is essential. Treatment is with Vitamin D3 and high dose calcium [6].
The natural evolution of malignant infantile osteopetrosis is death early in the first decade of life; without treatment survival after two years of age is rare. So far, there is no curative medical treatment, hence supportive treatment aimed at treating complications is offered. Bone marrow transplantation is the only effective treatment to halt the progression of the disease, which is reserved for the most severe forms. Genetic counseling should be done in all cases since it is an autosomal recessive inherited disease.
Conclusion
A multidisciplinary approach to Malignant Infantile Osteopetrosis is a priority. It is essential that the radiologist recognizes this entity to achieve a correct and timely diagnosis. The diagnosis of rickets superimposed on osteopetrosis is crucial as its treatment improves the general well-being of the child. General radiography has an important role in the diagnosis.
References
- Vomero A, Tapie A, Arroyo C, Raggio V, Peluffo G, et al. (2019) Malignant infantile osteopetrosis. Rev Chil Pediatr 90: 443-447.
- Gonen KA, Yazici Z, Gokalp G, Ucar AK (2013) Infantile osteopetrosis with superimposed rickets. Pediatr Radiol 43: 189-195.
- Rao PT, Sunita V, Gandhi TP (2013) Infantile or malignant osteopetrosis: Case report of two siblings. J Clin Diagnos Res 7: 1759.
- Olgaç A, Tümer L, Boyunağa Ö, Kızılkaya M, Hasanoğlu A (2015) Diagnostic dilemma: Osteopetrosis with superimposed rickets causing neonatal hypocalcemia. J Trop Ped 61: 146-150.
- Stark Z, Savarirayan R (2009) Osteopetrosis. Orphanet J Rare Dis 4: 5.
- Umesh K, Rajesh J (2009) Osteopetrorickets-Osteopetrosis with rickets: A rare paradoxical association. Intern J Pediatr Neonatol 10: 1.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences