Disseminated Tuberculosis Masquerading as a Simple Neck Abscess: A Case Report
Benazir Begum and Jayasree Babu*
Published Date: 2025-04-12DOI10.36648/2572-5483.10.2.279
Benazir Begum and Jayasree Babu *
Department of Otorhinolaryngology, Sri Manakula Vinayagar Medical College and Hospital, Kalitheerthalkuppam, Pondicherry, India
*Corresponding Author:
- Jayasree Babu
Department of Otorhinolaryngology, Sri Manakula Vinayagar Medical College and Hospital, Kalitheerthalkuppam, Pondicherry, India
E-mail:benazir25296@gmail.com
Received date: September 21, 2024, Manuscript No. IPJPM-24-19683; Editor assigned date: September 24, 2024, PreQC No. IPJPM-24-19683 (PQ); Reviewed date: October 08, 2024, QC No. IPJPM-24-19683; Revised date: April 05, 2025, Manuscript No. IPJPM-24-19683 (R); Published date: April 12, 2025, DOI: 10.36648/2572-5483.10.2.279
Citation: Begum B, Babu J (2025) Disseminated Tuberculosis Masquerading as a Simple Neck Abscess: A Case Report. J Prev Med Vol:10 No:1
Abstract
Background: Pott’s spine with Pre-Vertebral Abscess (PVA) presenting as an anterior neck abscess is a rare clinical entity, which often gets misdiagnosed precluding early diagnosis and treatment.
Case presentation: An Adolescent male who presented with a painless anterior neck swelling which was not responding to routine conservative management. Further investigation of the abscess unveiled a PVA and tubercular degenerative changes of the C6 vertebra. The cervical vertebra (C-spine) changes were initially identified on the Computed Tomographic (CT) scan, which was further confirmed on a Magnetic Resonant Imaging (MRI) of the neck. The PVA secondary to the Pott’s spine had tracked anteriorly to form a painless swelling in front of the neck without any cervical symptoms. The treatment required multidisciplinary teamwork between neurosurgeons, radiologists, pulmonologist, and head and neck surgeons. The patient made a good recovery after initiation of anti-tuberculosis therapy with C-spine stabilization.
Conclusion: Undiagnosed cervical Pott’s spine can lead to fatal consequences due to proximity to neurovascular structures; hence always have a suspicion of C-spine involvement in tubercular neck abscesses. Mutli-disciplinary team involvement is needed in treating patients with Pott’s spine. C-spine stabilization and antitubercular therapy are the main stay of treatment.
Keywords
Neck abscess; Pott’s spine; Prevertebral abscess
Introduction
Extra-Pulmonary Tuberculosis (EPTB) accounts for 15-35% of the total tuberculosis cases. Tubercular lymphadenitis is the most common EPTB and TB spine contributes to 1% of all the tuberculosis cases. Prevertebral neck abscesses caused by Pott's spine are rare, but can occasionally extend to anterior neck abscesses. Early recognition of occult spinal tuberculosis is imperative to minimize the neurological consequences and residual spinal deformity. This case report aims to discuss key aspects of the presentation, the role of imaging of the neck in suspected cold abscess cases, and the necessity of multidisciplinary teamwork in managing an unusual clinical presentation with review of literature.
Case Presentation
A 15-year-old young male presented to our hospital with a month history of swelling in the anterior aspect of the lower neck, which was painless and not responding to the empirical antibiotics. There is a history of pulmonary tuberculosis to his father one year ago, which was treated and declared cured. However, our patient did not exhibit any features of pulmonary tuberculosis. There was no history of neck pain or restriction of neck movement. He had fever on the initial days of noticing the swelling, which was later subsided by taking medications.
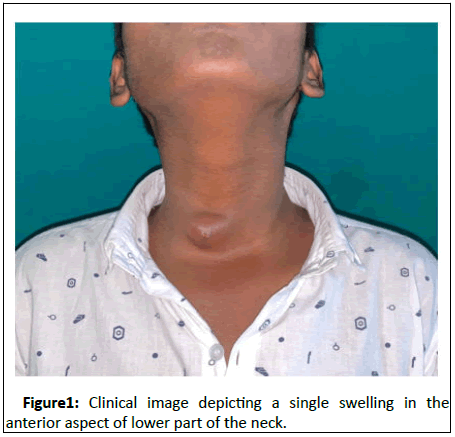
On examination, there was a single well-defined fluctuant swelling of size 3cmX3cm, not warm and non-tender, noted below the level of right lobe of thyroid gland. The swelling was not moving with deglutition or protrusion of tongue. The skin over the swelling had a pustular point, indicating the site of previous fine needle aspiration (Figure 1). The patient’s symptoms progressed despite medical treatment, with the recurrence of swelling post-aspiration.
Figure 1: Clinical image depicting a single swelling in the anterior aspect of lower part of the neck.
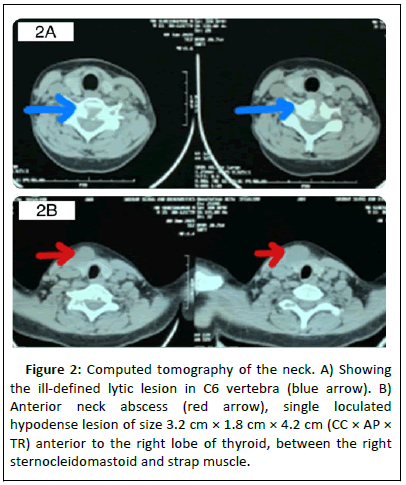
CT neck revealed a single loculated lesion anterior to the right lobe of thyroid (Figure 2A and 2B). MRI revealed partial destruction of C6 vertebral and an anterior pre-vertebral collection seen extending from the inferior endplate of C6 to D1 vertebra. A well-defined T1 hypointense, T2/STIR hyperintense collection noted in the right infrahyoid region anterior to strap muscles and both the lobes of thyroid which tracks posteriorly to communicate with the right C6-C7 neural foramina (Figure 3A and 3B).
Figure 2: Computed tomography of the neck. A) Showing the ill-defined lytic lesion in C6 vertebra (blue arrow). B) Anterior neck abscess (red arrow), single loculated hypodense lesion of size 3.2 cm × 1.8 cm × 4.2 cm (CC × AP × TR) anterior to the right lobe of thyroid, between the right sternocleidomastoid and strap muscle.
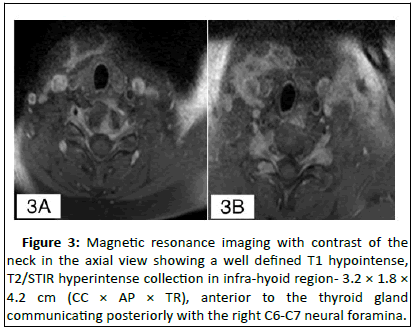
Figure 3: Magnetic resonance imaging with contrast of the neck in the axial view showing a well defined T1 hypointense, T2/STIR hyperintense collection in infra-hyoid region- 3.2 × 1.8 × 4.2 cm (CC × AP × TR), anterior to the thyroid gland communicating posteriorly with the right C6-C7 neural foramina.
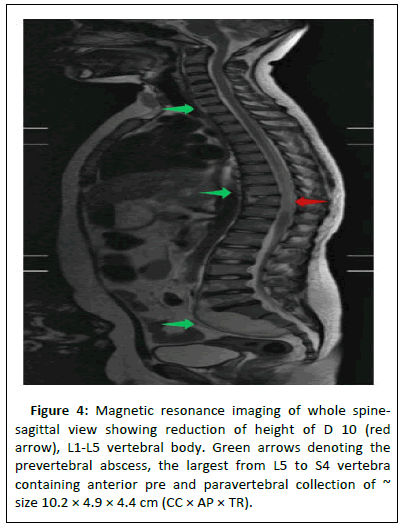
The ESR level was elevated and the Fine Needle Aspiration (FNA) sample sent from the swelling revealed no growth on cultures with a negative CBNAAT. Initially, the patient was suspected to have a suppurative bacterial lymphadenitis, which was ruled out with negative culture reports and abscess not responding to antibiotics. The first clue to Pott’s spine as the primary cause was revealed from the CT evaluation of the neck swelling (Figure 4).
Figure 4: Magnetic resonance imaging of whole spinesagittal view showing reduction of height of D 10 (red arrow), L1-L5 vertebral body. Green arrows denoting the prevertebral abscess, the largest from L5 to S4 vertebra containing anterior pre and paravertebral collection of ~ size 10.2 × 4.9 × 4.4 cm (CC × AP × TR).
The patient was treated by a multi-disciplinary team and was started on ATT based on the clinical suspicion despite negative CBNAAT report. He used Philadelphia collar for C-spine stabilization.
The patient was followed up serially over a period of one year. On the initial 2 week visit after the initiation of ATT, reduction in size of the neck swelling was noted followed by a complete reduction in swelling in six months. The patient was still advised to use hard-collar to the neck as the degenerative changes takes a longer time for recovery. Liver enzymes and urine analysis was done every month to exclude the presence of the ATT induced hepatitis and renal injury.
Results and Discussion
Tuberculosis (TB) is still one of the major causes of illness and death in developing countries like India [1].
The extra-pulmonary lesions often occur usually as a result of a primary focus of infection in the lungs with Mycobacterium tuberculosis. The lesions are often painless to begin with, enlarge and suppurate to form ulcers and sinus tracts in the overlying skin [2]. Our patient presented with painless suppurative swelling, which was suspected to be suppurative TB lymphadenitis as it is endemic in India. However, initial persistent fever, thick purulent pus on FNA and negative CBNAAT led to the diagnostic confusion. The sensitivity of CBNAAT in diagnosis of EPTB, from lymph node is 84.9%, hence if the test is negative, it is important to corroborate clinical findings, radiological features and histopathology features [3].
The typical symptoms of any forms of spinal TB that do not manifest with typical clinical and radiologic features of the disease are considered to be atypical spinal TB [4]. The spinal TB is perhaps the most dangerous atypical form of TB which can cause potentially fatal neurological consequences [5]. The cold abscess in spine develops slowly when tuberculous infection extends to adjacent ligaments and soft tissues with lack of pain and other signs of inflammation [6].
The evaluation C-spine in the suspected cold abscess of the neck is imperative even in the absence of neck pain or restriction of neck movements. MRI is the gold standard investigation for tubercular spondylitis which helps to identify the presence of an epidural component and cord compression [7]. In our patient, MRI helped to identify the extent of abscess and to delineate the tract between preverterbral and anterior neck abscess.
Multidisciplinary approach is crucial in the treatment of TBspine to facilitate early diagnosis and device a definitive management plan [8]. Spinal TB is a medical disease, however, in the presence of extensive abscess with imminent neurological compromise, surgical intervention might be warranted. Repeated aspiration in cold abscess can be an adjuvant to ATT, as it is a less invasive procedure and reduces the complications like sinus formation [9]. But, our patient had a prevertebral abscess which is extending to anterior neck; hence, repeated aspiration was not useful.
Conclusion
This case highlights the importance of considering disseminated tuberculosis in patients presenting with persistent or atypical neck abscesses. Early recognition and appropriate diagnostic evaluation are critical to prevent delays in treatment. Clinicians should maintain a high index of suspicion, especially in endemic regions or immunocompromised individuals, to ensure timely management.
Ethics Approval
Obtained from Institution Ethics Committee.
Consent
Written informed consent was obtained from the patient to publish this report in accordance with the journal’s patient consent policy.
Consent for Publication
Obtained.
Availability of Data and Materials
Consent for publication from the patient was obtained and data does not compromise anonymity or confidentiality or breach local data protection laws, for the dataset to be considered for publication.
Competing Interests
The authors declare that they have no competing interests.
Funding Sources
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Acknowledgement
N/A.
Author Contributions
BB was a major contributor in writing the manuscript.
JB (Corresponding author) was involved in reviewing and editing the manuscript.
References
- Yao M, Zhu ZH, Lian NF (2017) Treatment for 15 cases of cervical tuberculosis. Chin Med J (Engl) 130:1751–1752
[Crossref] [Google Scholar] [PubMed]
- Niblock AL (2011) Recurrent neck abscesses due to cervical tuberculous lymphadenopathy in an elderly woman post-splenectomy: a case report. J Med Case Rep 5:584
[Crossref] [Google Scholar] [PubMed]
- Arjun P, Nishal N, Arjun R, Ameer K, Nair S, et al. (2022) Diagnostic yield of CBNAAT in the diagnosis of extrapulmonary tuberculosis: A prospective observational study. Lung India 39:443
[Crossref] [Google Scholar] [PubMed]
- Rasouli MR, Mirkoohi M, Vaccaro AR, Yarandi KK, Rahimi-Movaghar V (2012) Spinal tuberculosis: diagnosis and management. Asian Spine J 6:294
[Crossref] [Google Scholar] [PubMed]
- Sinan T, Al-Khawari H, Ismail M, Ben-Nakhi A, Sheikh M (2004) Spinal tuberculosis: CT and MRI features. Ann Saudi Med 24:437–441
[Crossref] [Google Scholar] [PubMed]
- Garg RK, Somvanshi DS (2011) Spinal tuberculosis: a review. J Spinal Cord Med 34:440–454
[Crossref] [Google Scholar] [PubMed]
- Gambhir S, Ravina M, Rangan K (2017) Imaging in extrapulmonary tuberculosis. Int J Infect Dis 56:237–247
[Crossref] [Google Scholar] [PubMed]
- Lakhwani M, Raipure A, Seth N, Phansopkar P (2022) Impact of multidisciplinary approach in managing Pott spine–A case report. Med Sci 26:1
- Goswami R, Gangwani A, Shrivastava P (2019) Comparative clinico-pathological study of fine needle aspiration cytology and histopathology of various neck swellings in Bundelkhand region of Madhya Pradesh, India. Trop J Ophthalmol Otolaryngol 4:157–162
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences